Processing Medical Plastics? Here's How to Minimize Risk
FDA now expects OEMs of healthcare products to also take responsibility for Tier 2 and 3 suppliers—making sure every supply-chain link is meeting Good Manufacturing Practices.

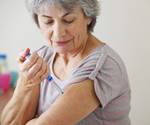
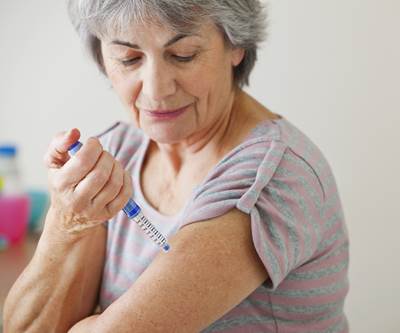
Plastics used in healthcare products like this inhaler much meet stringent quality and performance standards and also pass biocompatibility and biotoxicity tests.
In plastics processing for the medical and pharmaceutical industry, it’s all about risk. Or, better yet, about minimizing risk. Manufacturers of medical devices and pharmaceutical packaging, along with their customers, need to make sure there’s no chance a patient might have an adverse experience caused by some defect or oversight. Therefore, the companies supplying component parts also need to be vigilant to make sure actions they take don’t compromise the performance or safety of the final product.
Plastics used in healthcare provide vital functions such as enabling speedy diagnosis, minimal invasive surgery, self-medication, and reducing transmission of bacteria, as well as protecting drugs from moisture and oxygen. These materials must deliver consistent performance, including resistance to sterilization, chemicals and lipids. They often must also meet standards for biocompatibility and toxicity, where even slight changes in the ingredients in the plastics used could affect the acceptability of the finished device. For these reasons, regulatory authorities such as the U.S. FDA and relevant authorities in Europe require that the plastics are “well-characterized” with detailed information on the material ingredients and formulation, manufacturing processes, and extensive supporting data with respect to physical and mechanical properties, biocompatibility and toxicity.
The responsibility for assembling all this documentation ultimately falls to the company putting the device on the market as it becomes part of the package of data required to get the device approved for use. However, as regulators are increasingly scrutinizing risk of changes in the complete supply chain, the processor—Tier 1 as well as Tier 2 and 3 suppliers—has increased responsibilities for the plastic materials they are sourcing, even if specified by the OEM customer.
All of this argues loudly for collaboration between all parties in the supply chain, beginning early in the design process. Getting a medical device approved by the FDA and onto the market is complicated enough when everything goes smoothly and according to plan. The plastic part, and the ingredients that go into them, may represent a low cost per device, but, in the end, they play a vital role in the quality and reliability of the final device and thus could have a huge cost impact if there is a problem.
A plastics processor who understands the issue and who understands its role in the risk-management process can be a considerable asset to a medical or pharmaceutical manufacturer. Knowing the importance of change control, maintaining clear communication channels and investing in Good Manufacturing Practices (GMP) can go a long way in reducing risk for all concerned and make such a processor a valuable partner.
What is a Medical-Grade Polymer?
With very few exceptions, there are no true “medical-grade” polymers. In fact, almost any resin could be used in a medical application as long as it is “well-characterized,” and adequate controls on consistency are in place. This means that potential risks from the material have been assessed and it has been found to be acceptable.
Once these materials are properly documented, medical device manufacturers can use them in their designs and products with the confidence that they will meet regulatory and application requirements. However, the documentation is a point-of-time submission and is material- and formulation-specific. Any material or formulation change over the lifetime of the product, and at any point in a sometimes highly complex supply chain, can invalidate previous approvals.
It is at this point that “change control” becomes an important and formidable challenge. Any change anywhere along the supply chain—production site, process, specification, quality system, even minor ingredients—can have an impact on the characterization of the material.
The plastic parts, and the ingredients that go into them, play a vital role in the quality and reliability of the final device.
The FDA has been getting much tougher on the requirements for medical-device and pharmaceutical producers in terms of their responsibility for the supply chain. In the past, it was sufficient if the device manufacturers monitored their direct Tier 1 suppliers. They, in turn, were responsible to make sure their sub-suppliers were able to fulfill basic quality requirements. All the device manufacturer needed to do was confirm that proper audits had been completed and documentation was in order. That has all changed. Now the FDA says a medical device company or pharmaceutical company must also take responsibility for Tier 2 and 3 suppliers. They have to make sure that every link in the supply chain is fulfilling the overall GMP requirements in terms of change management.
This is why ISO 13485 certification is becoming more and more important, particularly since the FDA has proposed to harmonize the framework regulating system of this ISO standard. ISO 13485-2016 is the standard governing organizations involved in the design, production, installation and servicing of medical devices. If upstream suppliers, like plastics processors, are also certified to the standard, they provide their customers with the assurance that they have invested in and understand the medical-device risk-management principles that are core to the standard. Also, that quality control and testing procedures have been applied to the raw materials they use in the components they provide and that they have the documentation to prove it.
Likewise, just because a material has been used in past-generation devices does not mean it will be acceptable for a similar application in the future. It is highly unlikely that these materials have truly remained the same since the original design. The FDA has issued several guidelines on this topic.
What to Look for in Materials
Any material supplier that is serious about serving the medical/pharmaceutical market will have a thorough understanding of the end-use application requirements, medical-device regulations that OEMs must meet, risk-management practices, and they will have put change-control measures in place. Usually this involves enhanced GMP and probably certification to an advanced quality standard such as ISO 13485-2016.
Certain material suppliers have taken extra steps to produce portfolios of materials specifically for healthcare applications. Borealis, for instance, produces a dedicated range of polyolefins called Bormed, and Lyondell Basell makes a similar range under the Purell brand name. Others follow a similar path so that a fairly broad spectrum of polymers is available.
In the case of polymer production, although the grades destined for healthcare are produced in the same reactors, they are made under tighter quality controls, and come with a commitment of change notification, long-term supply and pre-testing against selected applicable healthcare regulations. When it comes to modifying polymers with color or additives, there is a much wider range of parameters and ingredients to control. Avient’s Mevopur product line, which encompasses both finished compounds as well as color and additive masterbatch concentrates, offers assurances similar to those offered by polymer producers named above. (Note: Avient is a new company formed by PolyOne’s acquisition of Clariant Masterbatches.)
Efforts are underway to better define what a “medical grade” plastic is or should be.
These sorts of procedures, and commitments are still exceptions, however. Not all production processes and specifications for materials are designed with change control in mind. For economic reasons, they are often subject to frequent changes, both major and minor, of ingredients such as pigments, stabilizers and lubricants. For this reason, careful sourcing procedures at each level of the supply chain are increasingly necessary to ensure that materials come with the necessary assurances, and that controls are in place.
There are efforts underway to better define what a “medical grade” plastic is or should be. VDI, the German association of engineers, has been working on such a standard and recently published it in German and English as VDI:2017. It only covers polymers, however, and since the polymers are often downstream modified (e.g. colored by masterbatch or compounded) and these modifications augment risk, the scope is perhaps too narrow.
MedPharmPlast Europe, which has a broad membership, and one of the few trade associations that is truly vertical, covering the complete supply chain of the medical and pharmaceutical market, is also working on a standard for medical-grade materials. It is expected to encompass elements from the VDI standard plus additional elements of downstream modification by compounding and concentrates.

As their use increases in medical and drug-delivery devices, it is important to remember that colorants and additives must be just as tightly controlled as the polymer.
What About Colorants & Additives?
Minor ingredients like colorants and additives may be precompounded into the polymer, or introduced in masterbatch form during molding or extrusion processing. While a great deal of care may go into decisions about the polymer to be used, these minor ingredients can be easily overlooked, which can cause problems down the road.
In fact, the FDA has previously suggested that colorants and additives should be regarded as “contaminants” in the polymer and thus they need to be just as tightly controlled as the polymer itself. Making the situation worse is the fact that decisions about these materials is often left to the processor. The device OEM may specify the primary material but then simply specify a color standard (e.g., Pantone, RAL), which is then sourced by the processor. Perhaps the molder or extruder might even select a colorant or additive that they have used in similar applications in the past, thinking it is “already proven.” This will not pass muster with the FDA, however. Their assumption is that something in the material will have changed over time and as such these minor ingredients need to be reassessed and fully documented.
The regulatory compliance and quality of a medical device or pharmaceutical packaging is only as good as its weakest link and that is why it is essential to ensure that nothing changes. Generally, pigment and additive substance suppliers do not give change notifications. Avient’s Mevopur team, for one, has instituted “fingerprinting” of incoming materials, to detect any changes.

This Lewiston, Me., compounding line, one of Avient’s three global production facilities of Mevopur medical-grade masterbatches and compounds, is segregated to reduce contamination.
ABOUT THE AUTHOR: Steve Duckworth is global head of marketing & business development for healthcare at Avient Corporation, a new company formed by PolyOne’s acquisition of Clariant Masterbatches. He joined Clariant in 2007 and was instrumental in launching the Mevopur line of “Controlled, Consistent and Compliant” color and additive masterbatch concentrates and polymer compounds used in the medical and pharmaceutical sectors. His global team works with manufacturers and their suppliers to minimize and manage risk while responding quickly to changing regulations. He is president and executive board member of the cross-industry group MedPharmPlast Europe and a member of its regulatory affairs committee.
Related Content
For Extrusion and Injection-Blow Molders, Numerous Upgrades in Machines and Services
Uniloy is revising its machinery lines across the board and strengthening after-sales services in tooling maintenance, spare parts and tech service.
Read More3D Printed Spine Implants Made From PEEK Now in Production
Medical device manufacturer Curiteva is producing two families of spinal implants using a proprietary process for 3D printing porous polyether ether ketone (PEEK).
Read MoreBMW Group Vehicle to Adopt 3D Printed Center Console
A vehicle coming to market in 2027 will include a center console carrier manufactured through polymer robot-based large-format additive manufacturing (LFAM).
Read MoreUS Merchants Makes its Mark in Injection Molding
In less than a decade in injection molding, US Merchants has acquired hundreds of machines spread across facilities in California, Texas, Virginia and Arizona, with even more growth coming.
Read MoreRead Next
Materials: Medical-Grade Compounds with Degradation Resistance and Enhanced for Laser Marking and Welding
Clariant is adding two new series to its Mevopur porfolio and marking its 10th year at MD&M West with the theme, The Color of Innovation – The Science of Design.
Read MoreWide Spectrum of Enhanced Medical-Grade Resins & Compounds Spotlighted at MD&M West 2020
Targeted at an impressive array of applications, the range of new medical-grade materials include modified PC copolymers, PEBA and TPUs, specialty copolyesters, a gamut of engineered compounds, and an advanced LSR.
Read More